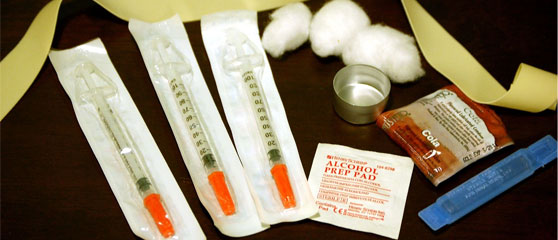
The lack of harm reduction measures for people who use drugs in UK prisons is fuelling health problems, including the spread of HIV and other infectious diseases. It’s time to introduce needle and syringe programmes.
We don’t tend to think about what it’s like to be a prisoner until the conditions of incarceration becomes an immediate reality in our own lives – whether it be the imprisonment of a friend, a relative, or even our own personal experience. Given that the general public have little contact with prisons, and perhaps little empathy for those who live behind bars, it comes as no surprise that the health and human rights of prisoners often falls short – particularly for one of the most vulnerable groups within prisons: people who inject drugs.
In 2012, the Home Affairs Committee reported that 70 per cent of incarcerated offenders in England and Wales reported “drug misuse” prior to imprisonment, 51 per cent reported drug dependency, and – according to the Ministry of Justice – “35 per cent admit injecting behaviour”. Given this evidence, it is essential for harm reduction practices, particularly needle and syringe programmes (NSPs), to be incorporated in prisons.
An NSP is a vital harm reduction tool available to the general population across England and Wales. The UK's National Institute for Health and Care Excellence describes the purpose of NSPs as "[reducing] the transmission of blood-borne viruses and other infections caused by sharing injecting equipment, such as HIV, hepatitis B and C". NSPs are most commonly accessed through pharmacies, or drug and alcohol services.
NSPs have been implemented in prisons abroad – including in Switzerland, Germany, and Spain – and have proven to be consistently successful in a "diverse range of prison settings", according to the Harm Reduction Coalition.
Despite this, NSPs have not be introduced in any UK prison, and controversy persists around their potential provision.
Without access to an NSP, people who inject drugs can only use needles that have been smuggled into the prison. Such equipment is far more likely to be infected, as the needles may be shared around several people, or used several times by the same person in unsanitary conditions.
The probability of becoming infected with HIV after using an infected syringe ranges from 0.34 per cent to 1.4 per cent, while the risk of being infected with hepatitis C ranges from 1.5 per cent to 5 per cent, according to DrugScope. The combination of these factors is why the provision of NSPs in prisons is so urgently needed.
The Prison Reform Trust reported in 2005 that rates of HIV and hepatitis C are “significantly higher” in UK prisons than among the general population. More recently, a 2015 study in England, published by the International Journal of Prisoner Health, concluded that "not providing sterile needles may increase risks associated with injecting for prisoners who continue to inject".
Although not focused on prisons, an extensive Australian study into the effectiveness of NSPs concluded that “there is compelling evidence that increasing the availability, accessibility, and both the awareness of the imperative to avoid HIV and utilization of sterile injecting equipment by [people who inject drugs] reduces HIV infection substantially”.
In 2009, plans to provide sterile needles to prisoners in Scotland were met with threats of a correctional staff walkout, amid concerns that needles would be weaponised against staff. Since then, despite the clear drawbacks of the status quo, British prisoners continue to be denied access to this fundamental aspect of harm reduction.
This lack of reform not only puts the health and lives of prisoners at risk, but also that of correctional staff who run the risk of being exposed to non-sterile needles. The increased rate of HIV infection also leads to an increased risk to both prisoners’ families and the broader public when prisoners are released back into the community.
Prisoners do not give up their human rights when they enter prison. Prisoners have the right to essential healthcare that ensures they do not leave sicker than when they arrived. The stigma against people who use drugs and prisoners must not obstruct their access to the same standard of care and human rights as the general public.